A painful, loose or infected hip implant deserves specialist revision from a revision hip replacement surgeon in Ahmedabad, not indefinite pain management. Revision hip replacement is among the most complex procedures in orthopaedics. It requires a surgeon with the specific experience, planning capability and implant systems that primary hip replacement simply does not demand.
Our specialist will call you within 2 hours
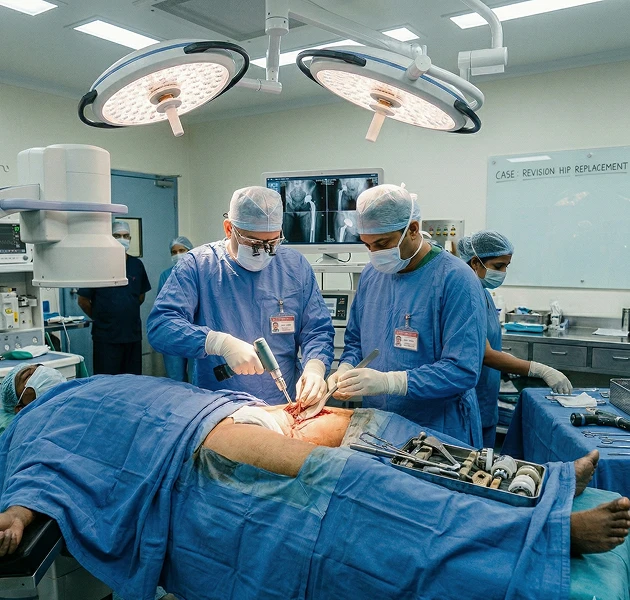
Revision hip replacement is a surgical procedure to remove and replace a failed, worn, loose or infected hip implant. It is considerably more demanding than a primary (first-time) hip replacement — the surgeon must work through scar tissue from the original surgery, manage bone loss caused by the failing implant, and use specialised revision implant systems designed to achieve stable fixation when the normal bone stock has been compromised. The outcome of revision surgery is directly determined by the experience of the surgeon, especially a revision specialist, and the availability of the right implant systems on the day.
The causes of hip replacement failure are varied — aseptic loosening (the implant working loose without infection) is the most common long-term cause, followed by periprosthetic joint infection (PJI), recurrent dislocation, bearing surface wear, and periprosthetic fracture. Each failure mode requires a fundamentally different surgical approach. Pre-operative assessment — CT scan for bone loss, infection markers (ESR, CRP, D-dimer), joint aspiration — is as important as the surgery itself. At Trayam Hospital, every revision hip case is assessed by our specialist team, including a revision hip replacement surgeon in Ahmedabad, with a full investigation protocol before any surgical decision is made.
If you have had a previous hip replacement and are experiencing these symptoms, a specialist review for hip revision surgery is recommended.
Revision hip replacement demands a different level of expertise, planning and implant availability, and the choice of centre matters.

Senior Consultant — Joint Replacement & Revision Orthopaedic Surgery, Trayam Hospital
Dr. Parth Patel has performed over 400 revision HIP replacement procedures — from straightforward single-component revisions to complex two-stage infected implant revisions with severe acetabular bone loss reconstruction. Revision HIP surgery demands a surgeon who has seen the full spectrum of failure modes, who approaches each case with a detailed pre-operative plan and who has the implant systems available to handle what is found once the joint is open. Every revision HIP patient at Trayam receives a personal consultation with full review of imaging and investigation results before any surgical decision is made.
The revision approach is determined by the cause and extent of failure — each scenario requires a distinct surgical strategy
A step-by-step guide to your recovery after Revision HIP Replacement at Trayam Hospital.
Surgery completed. Physiotherapy begins — first assisted standing and walking with a frame. Close monitoring of wound, blood count and inflammatory markers. Pain managed with multimodal analgesia protocol.
Hospital discharge for straightforward aseptic revisions. Two-stage septic revision patients remain for IV antibiotic management before oral transition. Walking with frame. Wound review at day 5–7.
Wound review and suture removal. Home physiotherapy programme established. Swelling and bruising reducing. HIP precaution restrictions in place — reviewed at 6-week appointment.
Outpatient review with X-ray confirming implant position and early bone ingrowth. Most patients walking with a stick or unaided. HIP precautions lifted. Driving discussed.
Significant improvement in pain and function compared to pre-revision. Most daily activities resumed. Physiotherapy continuing with strength and balance emphasis.
Full functional recovery for most patients. Return to recreational activity. Annual follow-up X-ray lifelong — essential for revision patients to monitor implant stability and detect early bone changes.
The most persistently under-investigated problem in HIP replacement in India is the patient with a failing implant who is repeatedly reassured that their X-ray looks normal. Plain X-rays miss acetabular cup migration, early osteolysis and subtle loosening that is clearly visible on CT. A patient whose replaced HIP is painful, unstable or showing progressive functional decline deserves a systematic investigation — not another steroid injection and a 3-month review appointment.
Revision surgery pricing varies significantly with complexity and implant requirements. We provide a fully itemised estimate — surgery, implant systems named and specified, stay and rehabilitation — before you commit. No flat revision package that may not cover what is found intraoperatively.
We will tell you if your HIP replacement pain can be managed without surgery. We do not recommend revision unless investigation confirms a clear, treatable cause of failure. An honest second opinion — even if the answer is that revision is not yet needed — is always available.
Revision HIP replacement is covered under most major health insurance policies. The complexity and specific implant requirements are documented correctly in the pre-authorisation submission. Our insurance desk manages this process in full — no inflated billing, no misrepresentation.
Painful HIP replacement? Dislocating? Old implant? You deserve a proper investigation by a revision specialist, not another injection.
Confidential · No Obligation · Reply in 2 Hours
Revision HIP replacement removes and replaces a failed, worn, loose or infected HIP implant. It is more complex than primary HIP replacement, requiring specialised implant systems, specific surgical training and thorough pre-operative investigation to determine the cause of failure.
Signs include: pain that never resolved or has returned after a period being well, recurrent dislocation, warmth and swelling suggesting infection, X-ray showing a shifted implant, noticeable leg length difference, or progressive functional decline. Any of these warrants specialist review.
Typically 2–3 hours for straightforward single-component revisions; 3–4+ hours for complex revisions with significant bone loss reconstruction — longer than primary HIP replacement due to scar tissue, bone loss management and larger revision implant systems.
Stage 1: implant removal, debridement of all infected tissue, antibiotic cement spacer. 6–8 weeks of targeted antibiotics. Stage 2: re-implantation once blood markers confirm infection clearance. Two-stage revision achieves over 85% infection eradication — the gold standard for established HIP PJI.
Straightforward aseptic revision: 5–7 days. Two-stage septic revision: stage 1 approximately 7–10 days; stage 2 approximately 5–7 days. Complex reconstructions may require longer depending on bone grafting requirements.
Yes — recurrent dislocation after HIP replacement has identifiable causes that are surgically correctable. Cup repositioning, use of a larger femoral head, constrained liner or soft tissue reconstruction addresses the specific cause. Revision for recurrent dislocation has high success rates when the correct diagnosis is made pre-operatively.
Longer than primary replacement — most patients reach functional recovery by 3–6 months. Complex reconstructions with significant bone grafting may take 9–12 months. Annual lifelong X-ray follow-up is essential for all revision patients.
Yes — covered by most major Indian health insurance policies and PMJAY. We manage pre-authorisation ensuring that the complexity and implant requirements are correctly documented and claimed in full.
Bring your X-rays, any existing reports and your surgical history. Our revision specialist will give you an independent, honest assessment of your options — and tell you clearly whether revision is needed and what it involves.