Severe shoulder arthritis, rotator cuff arthropathy and complex fractures treated by a shoulder replacement surgeon in Ahmedabad can destroy shoulder function. Shoulder joint replacement, total or reverse, restores pain-free movement when other treatments have failed. Return to everyday arm movement just weeks after shoulder joint replacement.
Our specialist will call you within 2 hours
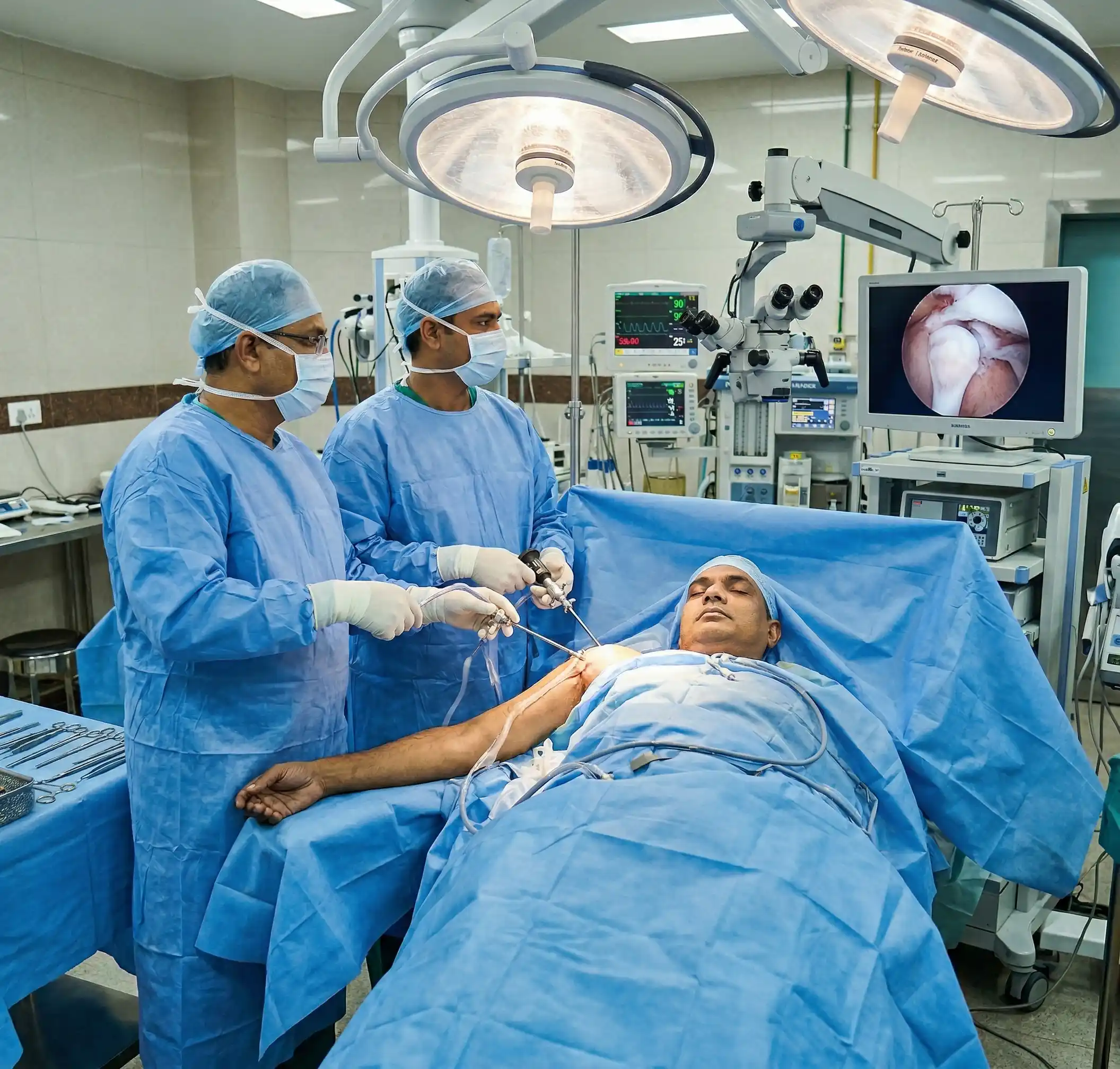
Shoulder replacement — shoulder arthroplasty — is a surgical procedure in which the damaged surfaces of the shoulder joint are replaced with artificial implants. The shoulder joint is a ball-and-socket joint: the humeral head (ball) sits in the glenoid (socket). In total shoulder replacement, both surfaces are replaced. In hemiarthroplasty, only the humeral head is replaced. In reverse shoulder replacement — the most important development in shoulder surgery of the past two decades — the ball and socket positions are deliberately swapped, allowing the deltoid muscle to take over the function of a destroyed rotator cuff.
At Trayam Hospital, shoulder replacement is performed using the latest implant systems with a minimally invasive deltopectoral approach — preserving as much muscle as possible, reducing blood loss and accelerating recovery. The implant type is selected based on the patient’s diagnosis, rotator cuff status, bone quality and age. Most patients notice dramatic pain relief within the first few weeks and achieve functional use of the arm within 6 weeks. Implant lifespan for modern shoulder replacements is 15–20 years with appropriate activity.
If you're experiencing any of these symptoms, a consultation with a shoulder replacement surgeon is recommended
Shoulder replacement is a subspecialty procedure — outcomes depend on correct implant selection, surgical technique and rehabilitation

Senior Consultant — Shoulder, Elbow & Upper Limb Surgery, Trayam Hospital
Dr. Parth Patel has extensive experience in both total and reverse shoulder replacement — including primary shoulder arthroplasty for arthritis and cuff arthropathy, revision shoulder replacement and shoulder replacement for complex proximal humerus fractures. The surgical approach at Trayam is built on thorough pre-operative planning with CT imaging, correct implant selection based on diagnosis, and a structured post-operative rehabilitation programme — the three factors that consistently determine shoulder replacement outcomes.
The right shoulder replacement depends entirely on your diagnosis, rotator cuff status and bone quality — not a one-size-fits-all approach
Surgery completed. Arm in a sling. Physiotherapy begins within 24 hours — pendulum exercises and gentle passive range of motion. Pain well-managed with multimodal analgesia. Most patients discharged day 3–4.
Sling worn continuously except for exercises. Passive and active-assisted range-of-motion exercises at physiotherapy. Portal or incision wound reviewed at 10–14 days. Desk work possible from week 2–3.
Sling progressively weaned. Active shoulder movement exercises commencing. Swelling and bruising resolving. Most patients can perform basic daily tasks — eating, grooming, dressing — without significant difficulty.
Active range of motion restoring. Strengthening exercises beginning. Return to light daily activities and driving (non-dominant arm at 6 weeks; dominant arm at 8–10 weeks). Shoulder feeling increasingly comfortable.
Most daily activities fully resumed. Progressive strengthening continuing. Pain levels dramatically reduced compared to pre-operative state. Return to light recreational activity.
Full functional recovery. Return to swimming, golf and recreational activity. Annual follow-up X-ray recommended to monitor implant and glenoid fixation — important for long-term implant surveillance.
The single most important decision in shoulder replacement surgery is choosing between total shoulder replacement and reverse shoulder replacement — and this choice hinges entirely on the status of the rotator cuff. Performing an anatomic total shoulder replacement in a patient with a significantly deficient rotator cuff leads to early failure — the implant destabilises without the cuff to control it. Yet this mismatch occurs regularly when the operating surgeon does not perform both procedures routinely and the pre-operative assessment of cuff status is inadequate.
Fully itemised estimate — surgery, implant type (total or reverse, named), stay, physiotherapy and follow-up — in writing before you book. You know exactly what is being implanted and why before you agree.
Total shoulder replacement when the cuff is intact. Reverse when it is not. The decision is made on MRI and CT findings — not on what is routinely stocked or what generates the highest margin.
Both total and reverse shoulder replacement are covered by most major Indian health insurance policies. Our insurance desk manages pre-authorisation with correct documentation of the indication and implant system used.
Severe shoulder pain or stiffness? Get an honest assessment of whether shoulder replacement is the right next step.
Confidential · No Obligation · Reply in 2 Hours
Total shoulder replacement replaces both the ball and socket in their anatomic positions — requires an intact rotator cuff to function. Reverse shoulder replacement swaps the positions — allowing the deltoid to drive shoulder elevation independently of the cuff. Reverse is used for cuff-deficient arthropathy, massive irreparable tears and selected fractures.
Total shoulder replacement: approximately 1.5–2 hours. Reverse shoulder replacement: approximately 1.5–2.5 hours. Total theatre time including preparation is approximately 30 minutes longer.
Most patients are discharged in 3–4 days — including the day of surgery, post-operative monitoring and initial physiotherapy before discharge.
Typically 4–6 weeks — the sling protects the soft tissue repair and allows early healing before active movement begins. The sling duration is not a reflection of surgical difficulty but of tissue healing timelines.
Basic daily tasks — eating, grooming — from week 3–4. Driving from 6–10 weeks depending on which arm. Overhead activity and lifting from month 3–4. Full activity at 6–12 months.
Modern shoulder replacements last 15–20 years in most patients. Glenoid component loosening is the most common long-term failure mode in anatomic TSA. Annual follow-up X-ray is recommended from year 5 onwards.
Risks include: infection (under 1%), glenoid loosening (long-term), instability, stiffness, nerve injury (rare) and implant wear. Reverse shoulder replacement has a higher dislocation risk than total shoulder in the early post-operative period — managed with sling protection and activity restriction.
Yes — both total and reverse shoulder replacement are covered by most major Indian health insurance policies and PMJAY. Our insurance desk manages pre-authorisation and cashless hospitalisation.
Talk to our shoulder specialist today. Bring your X-rays or MRI — or we arrange them. Book a consultation, no obligation.